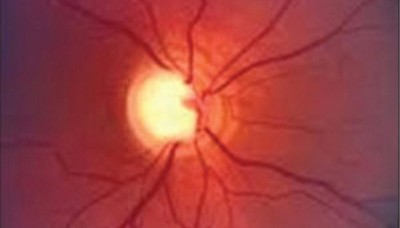
Glaucoma Awareness Month
There are approximately 3 million Americans who are living with glaucoma. Unfortunately, only about 50% of Americans know that they have glaucoma.
Read MoreSearch Our Website

There are approximately 3 million Americans who are living with glaucoma. Unfortunately, only about 50% of Americans know that they have glaucoma.
Read More
The top causes of visual impairments are refractive error, cataracts, and glaucoma, but just visiting the eye doctor can treat most of these.
Read More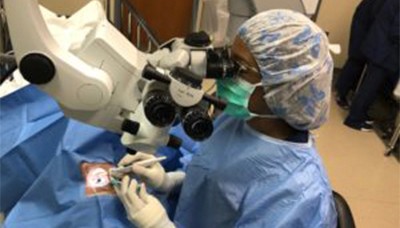
The iStent Inject is the smallest medical implant ever approved by the FDA. It is designed for open-angle glaucoma patients who need their cataracts removed.
Read More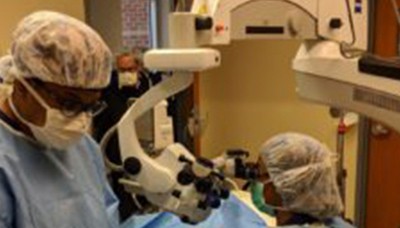
Dr. Constance Okeke performed the first Ab Interno Canaloplasty (or ABiC) glaucoma surgery in Hampton Roads.
Read More
Here's what our doctors at Virginia Eye Consultants have to say about Dr. Constance Okeke’s new book “The Building Blocks of Trabectome Surgery: Patient Selection.”
Read More
Dr. Constance Okeke’s new book “The Building Blocks of Trabectome Surgery: Patient Selection” shares her extensive experience pioneering micro-incision glaucoma surgery (MIGS)
Read More
Our ophthalmologist Dr. Constance Okeke emphasizes one type of solution in particular that has provided advanced potential in the scope of glaucoma treatment.
Read More
Laser treatments and surgery can both provide great results for helping control glaucoma, while reducing or eliminating the need for eye drops.
Read More
If you’ve been diagnosed with glaucoma, there’s a good chance you have been prescribed medicated eye drops to help keep the condition from progressing.
Read More
Our eye care specialists at Virginia Eye Consultants strive to offer our patients the benefits of the latest technology and techniques.
Read More
Virginia Eye Consultants’ board-certified ophthalmologist Dr. Constance Okeke recently completed two new glaucoma surgical procedures: a TRAB360 and a VISCO360.
Read More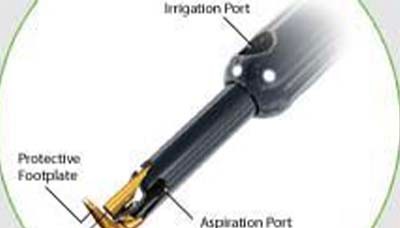
Dr. Constance O. Okeke is the first certified Trabectome surgeon in Hampton Roads, making VEC the only practice in the area to offer this advanced glaucoma treatment.
Read More
Dr. Okeke of Virginia Eye Consultants is the first ophthalmologist in Hampton Roads to perform the Glaukos iStent procedure.
Read More
Given the great importance most of us place on sight, it would seem to follow that we’d give them the best care possible, but sometimes we get too busy or we forget...
Read More
We are celebrating yet another advancement and achievement by our very own Glaucoma specialist, Dr. Constance Okeke, MD, MSCE. Dr. Okeke, being no stranger to both laser catar
Read More
We are celebrating yet another advancement and achievement by our very own Glaucoma specialist, Dr. Constance Okeke, MD, MSCE
Read More